OUR MISSION
The Maternal, Newborn, Child, and Youth Network works to realize our vision of :
The Maternal, Newborn, Child, and Youth Network works to realize our vision of :
 Improve Health Outcomes
Improve Health Outcomes
 Better Operational Management
Better Operational Management
 Seamless Systems Integration
Seamless Systems Integration
 Enhanced Learning & Growth
Enhanced Learning & Growth
The purpose of the MNCYN is to support the consistent delivery of safe, quality maternal, newborn, child, and youth care across our region. We achieve this by promoting and advocating for a consistent standard of care.
Our Network is seen as adding significant value through its ability to:
MNCYN fulfills its mission by offering a number of deliverables and services in our geographical region in Ontario to help healthcare organizations meet their objectives and exceed professional regulations.
Deliverables:
 Deliverables will be defined by the strategic Plan which is developed every three years through a strategic planning session and vetted by the Regional Steering Committee and the Executive Committee.
Deliverables will be defined by the strategic Plan which is developed every three years through a strategic planning session and vetted by the Regional Steering Committee and the Executive Committee.
 Strategic initiatives will be defined and working groups established.
Strategic initiatives will be defined and working groups established.
 Metrics will be developed, measured and reported out to our regional partners.
Metrics will be developed, measured and reported out to our regional partners.
Services:
 Case & Critical Events Reviews
Case & Critical Events Reviews
 Site Visits & Consultations
Site Visits & Consultations
 Workshops, online orientation programs, tools and documents
Workshops, online orientation programs, tools and documents
More information on our Services and Core Business Deliverables can be found on our Membership Benefits page.
Claire Martin
Kristine Fraser
Gwen Peterek
Kendra Savage
Stacy Laureano-Steele
Dr. Kevin Coughlin
Dr. Jordan Schmidt
Dr. Henry Roukema
Dr. Paige Burgess
Dr. Rahul Ohja
Dr. Roderick Lim
Meagan Furnivall

Our logo stylishly depicts the progression of newborn, child and youth in a maternal embrace. It represents a strong sense of confidence, community and cultural diversity emblematic of Canadian society.
The logo speaks to the creativity, cooperation and professionalism required of such an organization. Modern and dynamic, it symbolizes the collaboration and positive partnerships that the MNCYN strives to achieve for the regional health care sector.
A strategic planning session is held every three years with our regional partners and key stakeholders. The strategic priorities are determined by the feedback (themes) as voiced by our partners. The themes are then positioned under the strategic pillars of MNCYN, Quality Health Outcomes, Systems Integration, Improved Asset Management and Enhanced Learning and Growth.
The MNCYN strategic plan is a living document that is frequently revisited and updated as required to ensure our priorities are relevant, aligned with public health care outcomes and meeting the needs of our partners.





Established in 1979 at St. Joseph’s Hospital, London, Ontario, the Program was the vision of Dr. Graham W. Chance, a Neonatologist, who was born in Birmingham, England and educated in the UK. Dr. Chance immigrated to Canada in the 1970’s and spent his first years at the Hospital for Sick Children in Toronto, before coming to London, Ontario. A collaborative and multidisciplinary approach was undertaken, based on needs assessment, to provide perinatal education and support to 33 regional hospitals in the southwest catchment area.
The program focused on building relationships with the regional hospitals and promoting collaboration through the organization of district perinatal nurse leaders, as well as promoting standardized care through the development of standardized chart forms, maternal newborn education and the development of a regional obstetrics database to provide metrics by which to measure outcomes and benchmarking. Collaboration on a national level was realized with the creation of the Canadian Perinatal Programs Coalition (CPPC) in 1989.
A collaborative study conducted to determine the impact of the Outreach Program concluded that perinatal care in southwestern Ontario is regionalized and not centralized. The final report, “Is Perinatal Care in Southwest Ontario Regionalized?”, was published in 1991 (CMAJ).
With challenges faced by Regional hospitals due to economic recession, funding cuts, nursing staff layoffs and hospital amalgamations, the Perinatal Outreach Program maintained ongoing support and was identified by the Ministry of Health in a provincial maternal newborn care survey to be an exemplary model for ongoing education in perinatal matters. Regional and provincial collaboration were also continued through the establishment of a Regional Perinatal Care Steering Committee (1998) and the Ontario Provincial Perinatal Partnership (OP3) to advocate for consistent and collaborative care between hospitals and community agencies, including CritiCall and Best Start.

The Southwestern Ontario Perinatal Partnership (SWOPP) (formerly Regional Steering Committee), initiated discussions around shared governance and the anticipated merging of all perinatal services at LHSC. An external review was undertaken (2007), which recommended that a shared governance model, funding and sustainability plan be assumed collectively by the member hospitals that formed SWOPP. Over the next several years the SWOPP was reorganized to become the Maternal, Newborn, Child & Youth Network (MNCYN), which included a new paediatric education component known as the Paediatric Advancement Program (2009).

In 2011 the city-wide merger of Perinatal and Women’s Health Programs (St. Joseph’s Health Care London & LHSC) was completed with Program moved to LHSC (June 2011).
MNCYN continued to promote collaboration regionally and provincially through participation on the Provincial Council for Maternal and Child Health (PCMCH) (2010), supporting initiatives such as the Southwestern Ontario Perinatal Capacity Assessment Study, funded by the Southwest LHIN, aimed at determining the levels of maternal-newborn care required to support the needs of the population in Southwestern Ontario, minimize acute transfers and foster care closer to home.
Several new initiatives were introduced, including development and implementation of core competencies and assessment tools for perinatal and paediatrics, and development and launch of a Regional Paediatric Orientation (RPO) Program.
MNCYN celebrated its 40th anniversary (2019).

Ministry of Health LHINs’ boundaries change and expand geographically. The former SW Ontario region will be known as “West Ontario”.
In order to achieve the best outcomes with the lowest possible cost to the system and to patients and families, an integrated, comprehensive, and coordinated provincial approach is required to change practices and drive improved quality and access across the province. To that end, a unified proposal was made by PCMCH and other key stakeholders including MNCYN, to the Ministry of Health to develop a “Network of Networks” that would include CMNRP, SOON, MNCYN, SOMCHN and, eventually, a North Network.
A MNCYN rebranding project, undertaken to reinforce regional shared governance of the Network, involved the launch of a new logo and website and transition of program names (Regional Perinatal Program and Regional Paediatric Program).
The MNCYN follow the Accountability & Operational Structure (shown below), with top priority being given to our patients and their families.
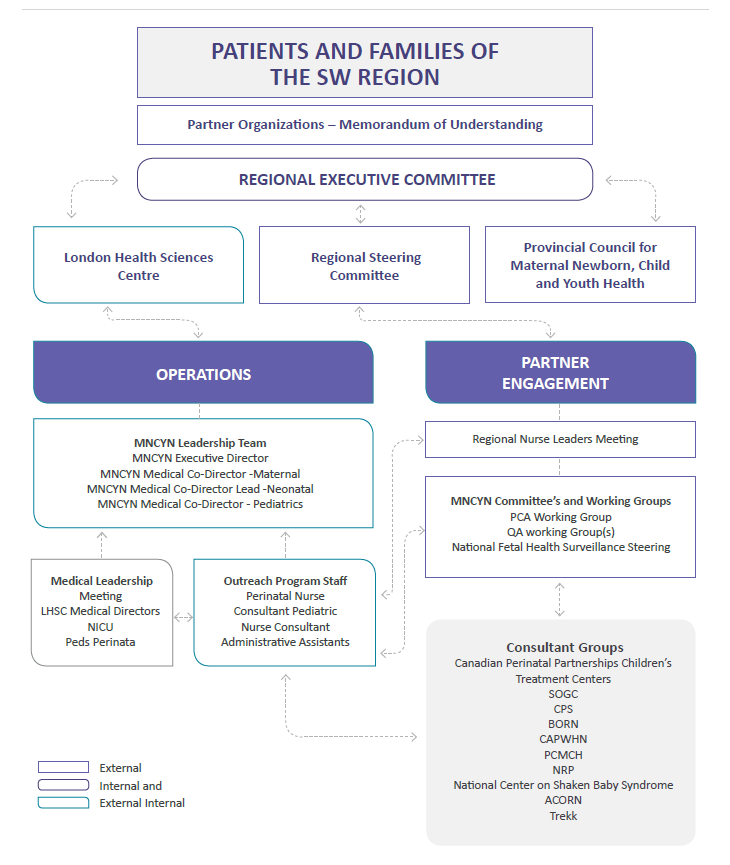
View PDF of the MNCYN Organizational Structure.
Reporting to the Partner organizations’ CEO/ Medical Officer of Health, the Network Regional Steering Committee will make strategic decisions as they apply to the Network and will plan for the successful evolution of program developments in Southwestern Ontario as agreed to by the Partners. The Regional Steering Committee will ensure that the key goals, vision and mission of the Network are consistent with the direction of the Ministry of Health and Long-Term Care, the Ministry of Health Promotion and the Ministry of Children and Youth Services, nationally recognized best practice standards, and the needs of The Partners and other stakeholders. Additionally, the Regional Steering Committee will review reports and recommendations resulting from the work of the Task and Working Groups. The Regional Steering Committee consists of one representative from each Partner organization.
In order to facilitate the operations and management of the Network, an Executive Committee will be formed to represent the Regional Steering Committee. The Executive Committee will report to the Regional Steering Committee at minimum semi-annually or more often when necessary.
MANDATE
The Executive Committee undertake the following responsibilities:
MEMBERSHIP
Membership is voluntary and will include the following:
Reporting to the MNCYN Regional Steering Committee, the Perinatal and Paediatric Educators Committee (PPEC) will coordinate efforts to support regionalized education for all partner organizations. This group will provide an opportunity to share resources, assist MNCYN in identifying educational and clinical skill gaps, and strategize to ensure equal access to education resources. As well, this PPEC Committee will support/participate in bi-annual nursing skills days in order to improve equal access to best-practice care across the region. The MNCYN Professional Practice Consultants will formulate agenda items prior to each meeting, with additions from the PPEC Committee.